- IVF and Female Infertility: Causes, Diagnosis, and Treatment
- IVF and Male Infertility: Causes, Diagnosis, and Treatment
- How To Prepare For IVF: Diet, Exercise, And Lifestyle Guide For IVF Success
- Comprehensive Guide to IVF Treatment in Turkey: Cost, Planning, Experience
- After IVF: Implantation, the 2-Week Wait, and Failure
You’ve made it to the 4th chapter! Now, you have a basic idea of what IVF is, and how it can treat male infertility and female infertility. Now, it’s time to look at data and studies to see how successful IVF is. The reason people choose to opt for IVF over other fertility treatments undoubtedly is the impressive results, as IVF is the most efficient and successful treatment available today. To properly understand IVF success rates, in this chapter we will go over;
- The IVF funnel
- IVF success rates
- Success rates of IVF for unexplained infertility, endometriosis
- Success rates of IVF types, other ART procedures, and their comparison
- Success rates of IVF with additional treatments, and how they can increase the chances of IVF working
When you finish this chapter, you’ll get a clear understanding of what IVF is capable of. The numbers will speak for themselves as to why people chose this procedure over others.
IVF Funnel
Our first step to understanding what IVF is capable of is to learn about the IVF funnel. You can think of this funnel as your personal success rate calculator. Regardless of other factors, your personal chance of success first and foremost depends on how many eggs you can produce.
As we have learned, during your natural cycle you produce 1 egg; and with ovarian stimulation, your ovaries are made to grow multiple eggs. These eggs are retrieved for fertilization. The average number of follicles retrieved for IVF is between 10 and 20. So, let’s go over a scenario where you produce 15 eggs, and how this number travels down through the IVF funnel.
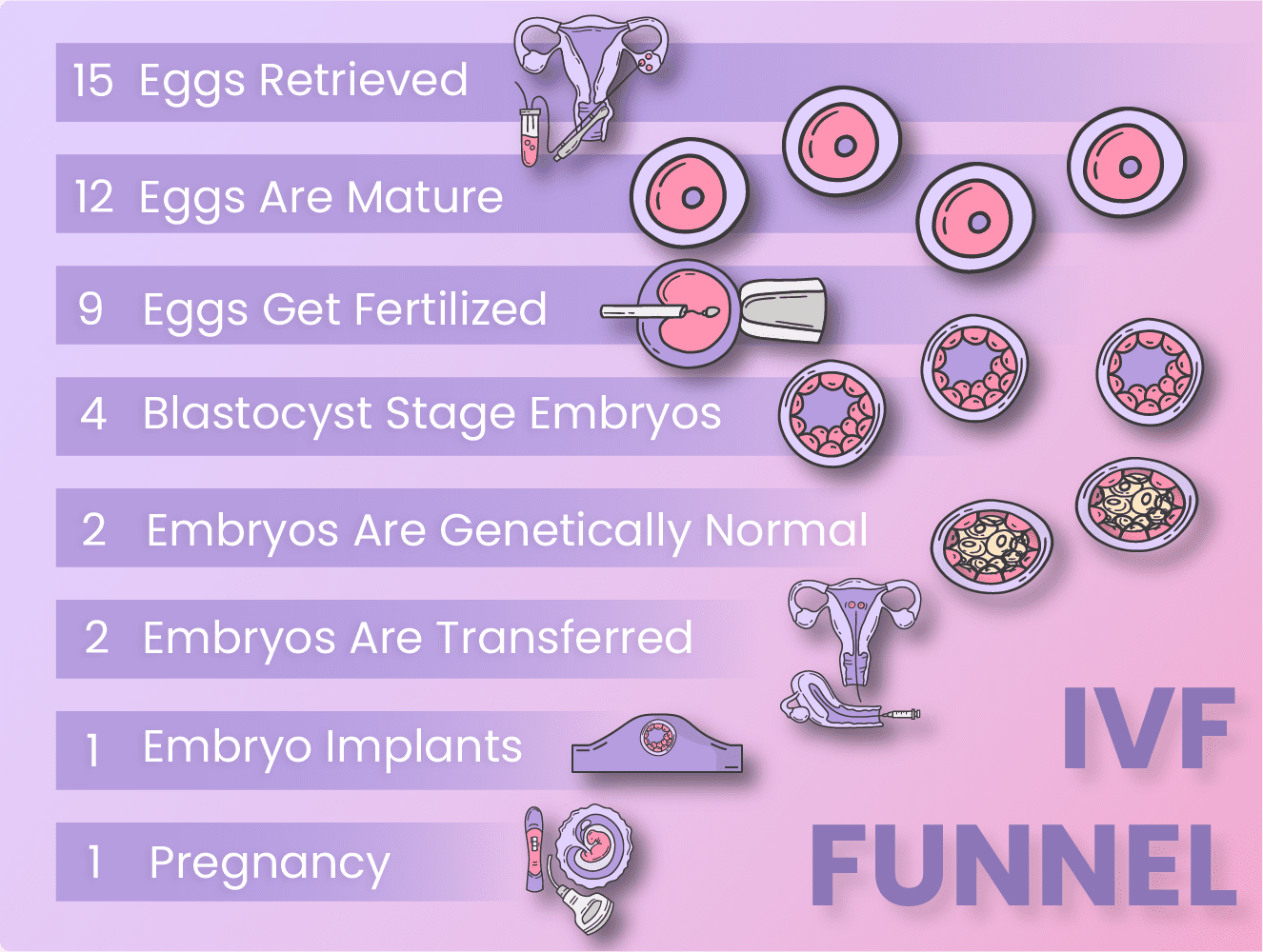
- During egg retrieval 15 eggs are retrieved. However, only 12 of these eggs are matured, meaning they’re at a stage where there can accept the sperm and get fertilized. Immature eggs cannot be fertilized. So from retrieval to the assessment of eggs for maturity, there has been a 20% decrease in the number of eggs.
- These 12 eggs are inseminated in vitro, and only 9 of them get fertilized. Sometimes, depending on the quality of the eggs or the sperm, fertilization can’t occur, even in optimized situations. So, we had 12 mature eggs, and now we are down to 9 fertilized eggs, which means that the IVF fertilization rate was around 60% for this cycle.
- From these 9 fertilized eggs, 4 of them reached the blastocyst stage. Not all fertilized eggs start their growth at the same time. Of these 4 embryos that reached to blastocyst stage, after embryo grading and PGT, only 2 of them ended up being genetically normal. So we went from 15 eggs to only 2 embryos that are available for implantation.
- These 2 genetically normal embryos are transferred into the uterus. Only 1 of them implants, and develops into a baby.
We started our journey with 15 eggs retrieved and ended up with 1 baby. So, how many follicles you produce, directly affects your chances of pregnancy. This is why the chance of pregnancy is very low with Natural IVF compared to the conventional protocol. Of course, this is an example scenario, and the numbers can change for different cases. However, IVF implantation rates, fertilization rates, and blastocyst rates are relatively similar among people of similar age groups and diagnoses.
So, does this mean that you should aim for as many eggs as possible? No, after a certain number, having more eggs than average doesn’t improve the chances of success. This also doesn’t mean that if the number of eggs retrieved is below average, pregnancy cannot occur. There are many factors that affect if you can get pregnant or not besides the number of eggs retrieved. Now let's look at some data regarding live birth rates in general. While the IVF funnel is useful for personal use, or what to expect, the main point of IVF is to have a healthy baby, which most data focuses on.
IVF Success Rate
For most of the charts presented, we used the data from the 2019 National Summary Report by Society for Assisted Reproductive Technology, unless stated otherwise. The numbers represent the live birth rates for patients going through all types of IVF cycles, including first and later cycles, and various additional treatments. So, keep in mind that we think of ‘IVF success rates' as all live birth rates. Also, live birth rates go up in most cases with each consecutive cycle. We will start with an overview of the success rates, and delve deeper into specific aspects; like comparing success rates of different stimulation protocols, different diagnoses, miscarriage rates, and adjunct treatments to IVF.
|
Age |
<35 |
35-37 |
38-40 |
41-42 |
>42 |
|
IVF live birth rate per |
55.0 % |
41.0 % |
26.8 % |
13.4 % |
4.3 % |
|
IVF implantation rate per |
51.2 % |
45.5 % |
35.7 % |
22.1 % |
8.7 % |
IVF Live Birth Rate
This is the general overview of the data presented to the public. This data includes IVF live birth rates for all cycle types and all additional treatments. The live birth rate is fairly high for people that are younger than 35. This is why considering IVF at a young age, or fertility preservation is so important. Younger female adults respond better to ovarian stimulation and have better quality oocytes, which also directly affects the embryo quality. We can also see the IVF funnel at play with the implantation rates. After the age of 40, live birth rates are almost half of the implantation rates. Let’s take a closer look at the effect of age on IVF. [1]
IVF Success Rates by Age
As we talked about before, age is the most important factor affecting fertility in women. After the age of 35, ovarian reserves and oocyte quality decrease significantly. If we remember the funnel model, this means that we will have fewer eggs to begin with, and most of them will be lost due to poor quality. Not only older patients will have difficulty with fewer, poor-quality eggs, but they will also have a difficult time during pregnancy. For patients over the age of 42, the miscarriage rate reaches 35%. This is because pregnancies over the age of 40 are considered high risk for both the baby and the mother, and IVF itself adds to this risk. [1]
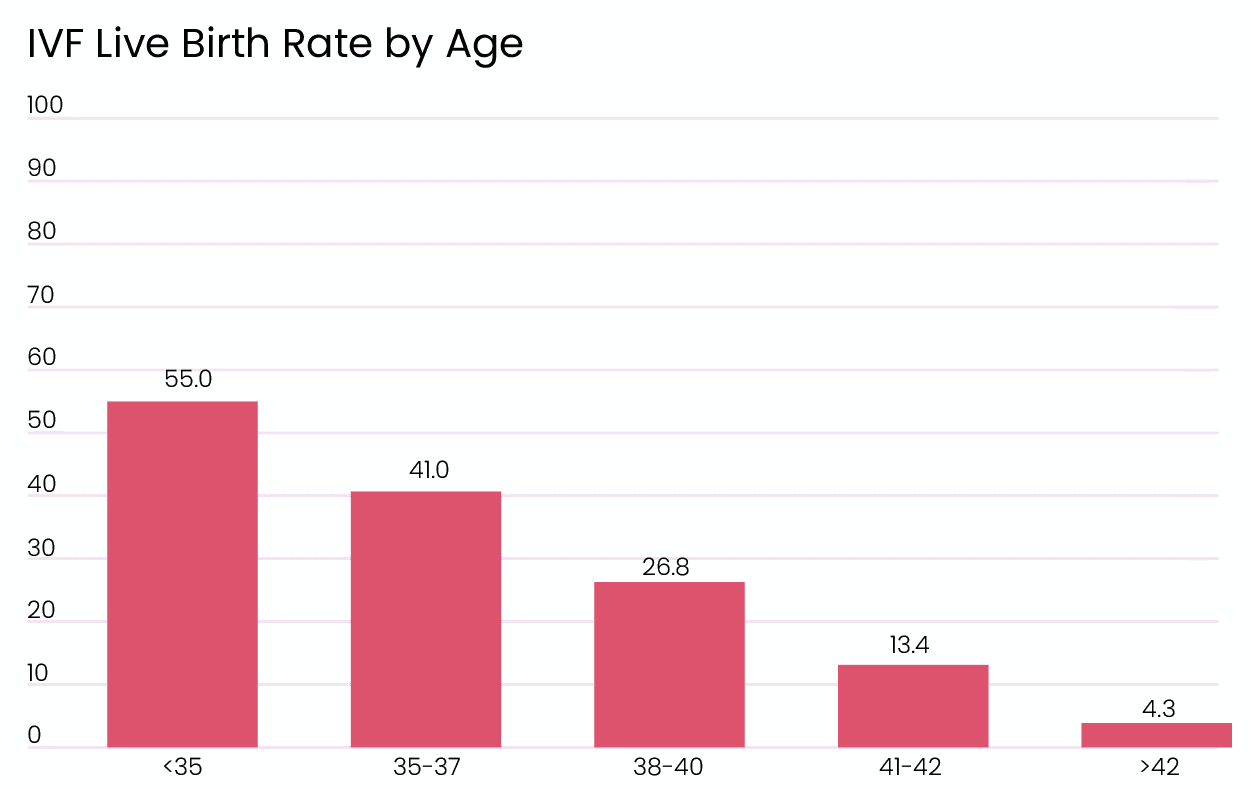
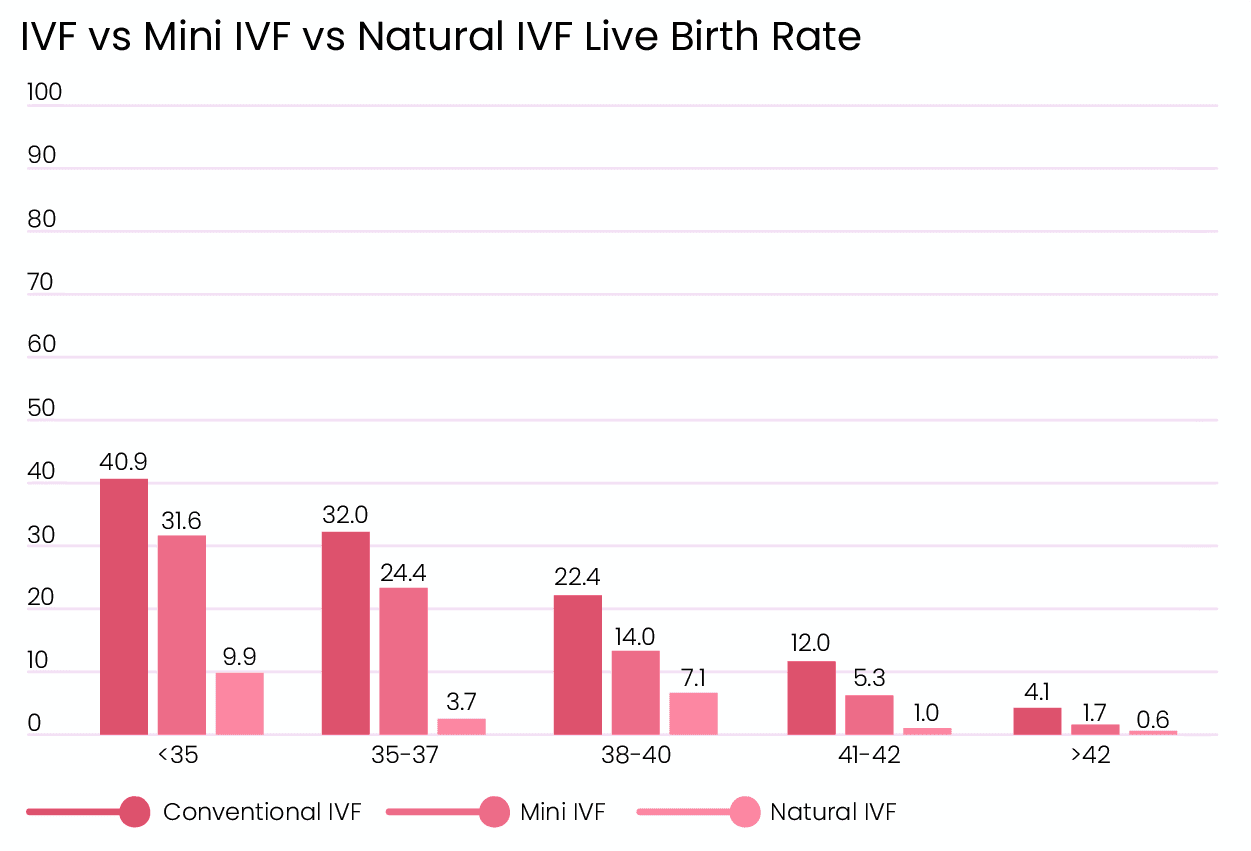
Natural IVF and Mini IVF Success Rates
When put in comparison, conventional IVF stimulation cycles have significantly higher live birth rates than mini and natural cycles. Ovarian stimulation allows doctors to retrieve more eggs, directly increasing the chances of success. Though conventional IVF results in more live births, it’s not suitable for everyone. Some patients have to go through minimal or no stimulation protocols for health reasons. But it’s important to be realistic about the expected results. [1]
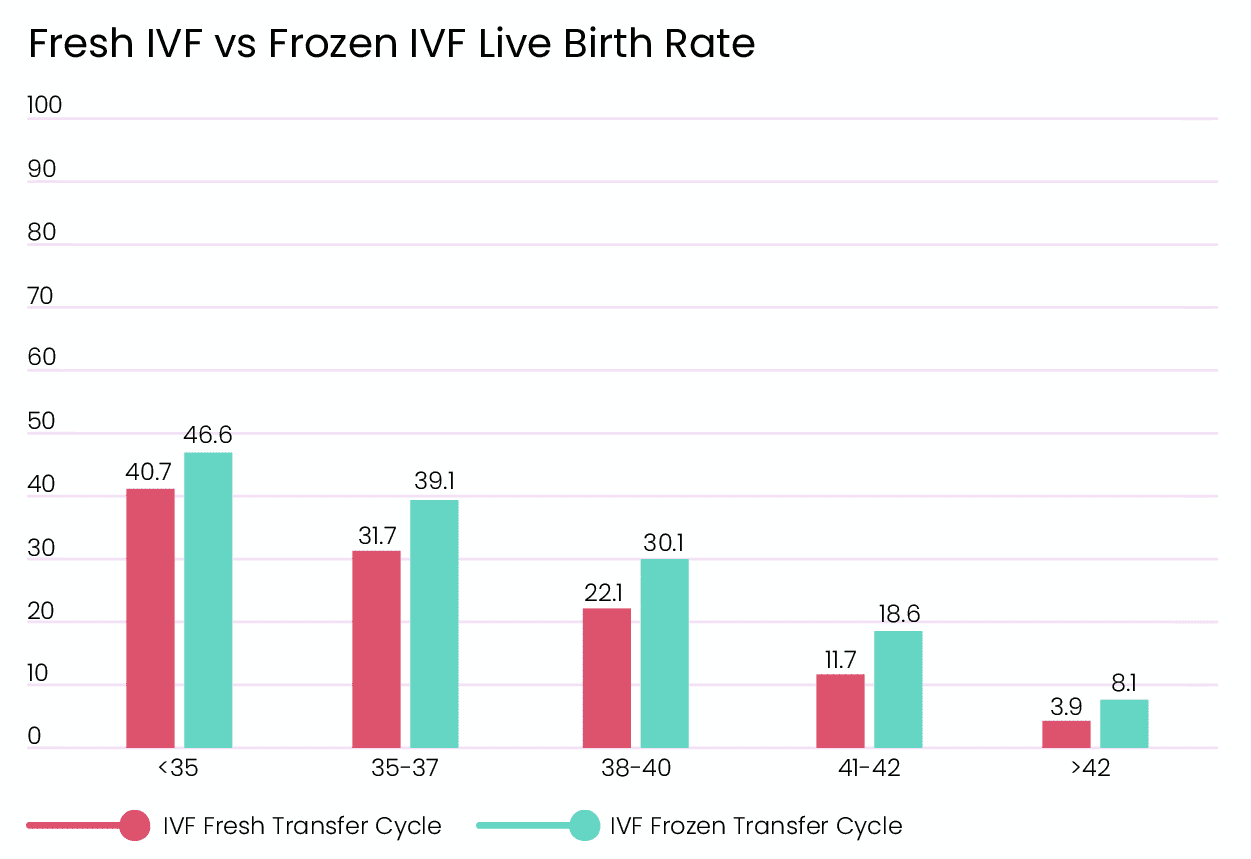
FET IVF success rates
Just as patients have questions about how different stimulation protocols affect success rates, they also have questions about if they should go with frozen transfer or not. The data presented here represents live births per egg retrieval for first-time embryo transfer. We can see that frozen embryo transfer can provide better results. This is because people can freeze their embryos at a younger age when they have better quality eggs, which will make good embryos in the future. Or, after the cryopreservation of embryos, patients can go through additional treatments that will optimize their uterine lining for implantation. [1]
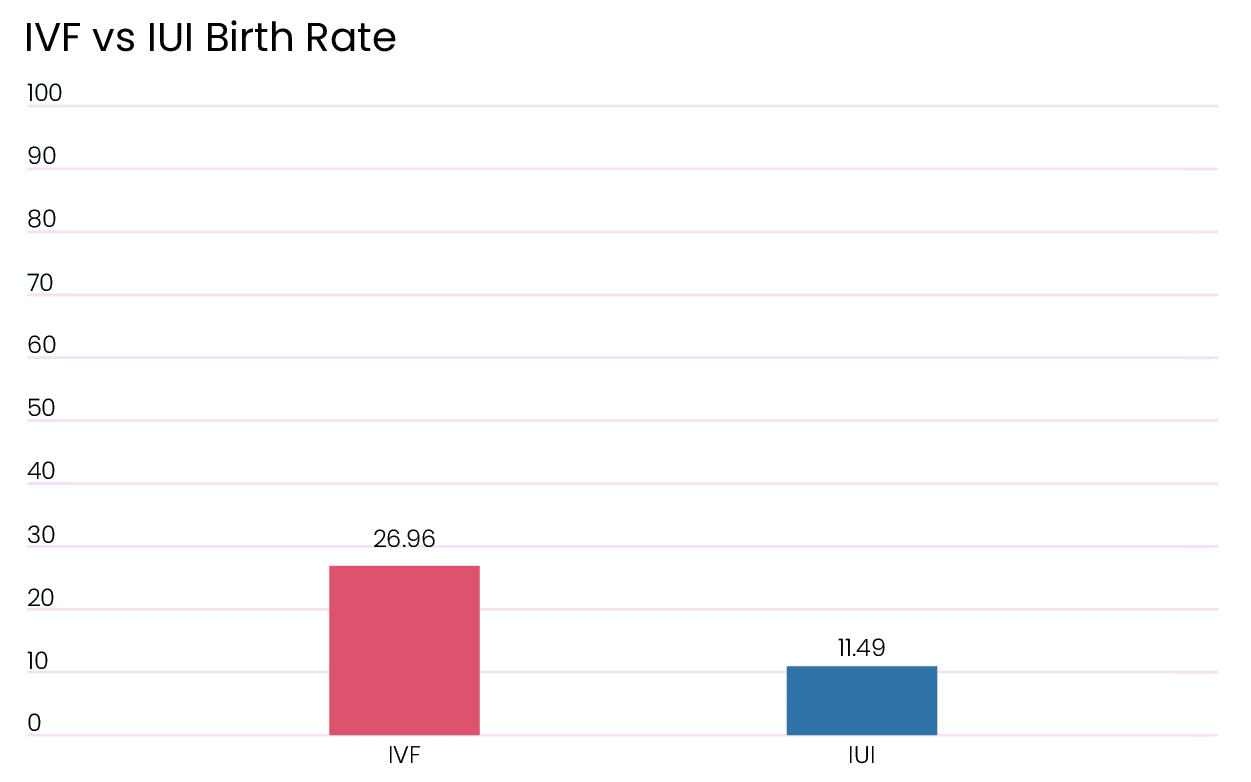
IUI vs IVF Success Rate
In a study done in the UK birth rates for IVF were also higher than for IUI [2]. The lower live birth rate for IVF in this study is because the success rates were not divided among age groups. However, a lower birth rate doesn’t mean that IUI is not useful. IVF provides better results, but it’s also more invasive. If there is reason to believe that a patient can get pregnant with IUI over IVF, that should be taken into account.
ICSI IVF Success Rates
ICSI is the most common adjunct procedure to IVF. ICSI revolutionized the world of fertility treatments, to say the least, and its very high fertilization and the live birth rate are what make it so popular. Let’s compare the live birth rates of IVF with and Without ICSI.
When IVF is combined with ICSI it yields significantly higher live birth rates. Between the age groups 38 to 42, ICSI nearly doubles live birth rates, and for women over the age of 42, their live birth rate triples. [1]
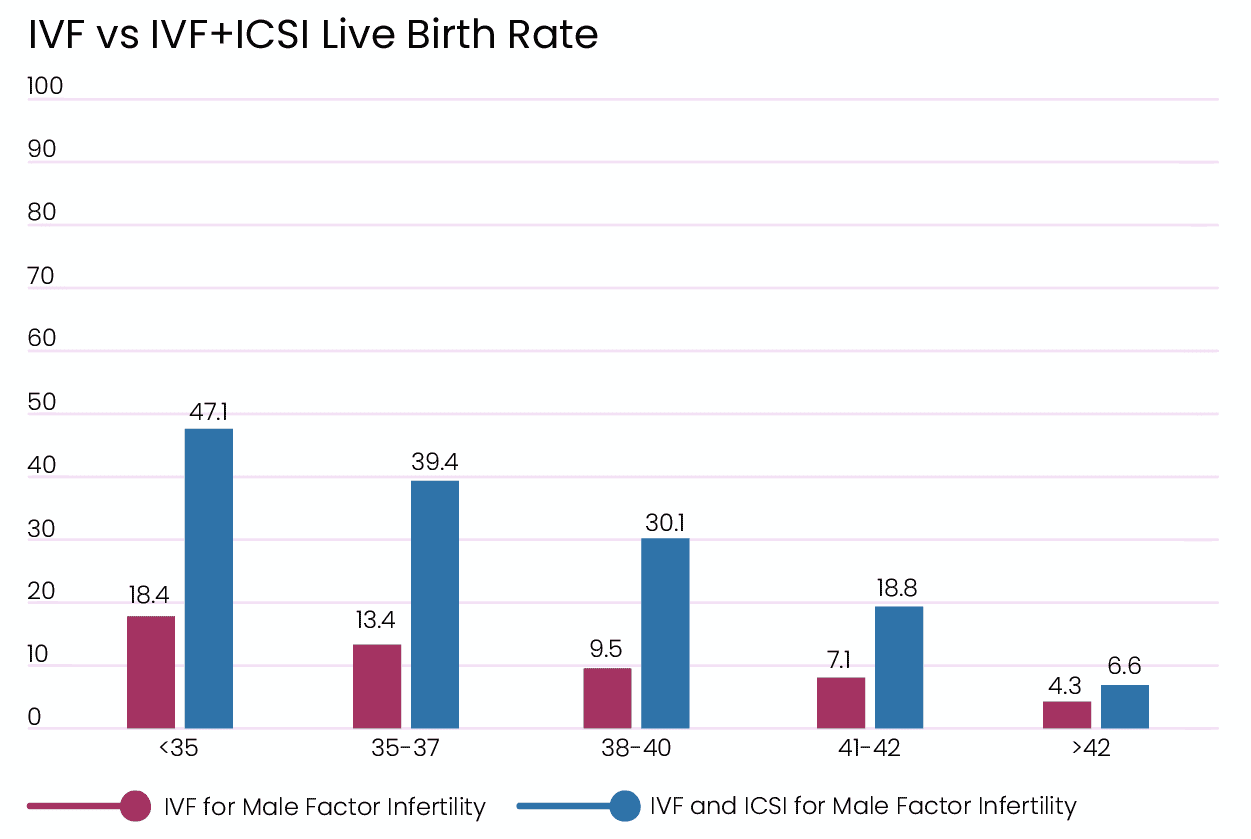
Even though ICSI is very common nowadays, and used in cases where the diagnosis might not be male factor infertility it was originally intended as a treatment for male infertility, and that’s where it shines. Let’s look at live birth rates for patients that have a male infertility diagnosis, and how IVF by itself compares to IVF and ICSI combined.
IVF by itself is not enough to treat male infertility. When combined with ICSI, IVF for male infertility treatment is three times more effective in most cases [1]. So, if you have a male infertility diagnosis, ICSI can significantly improve your chances of having a baby.
|
Age |
<35 |
35-37 |
38-40 |
41-42 |
>42 |
|
IVF with ICSI |
43.2 % |
34.4 % |
24.8 % |
13.5 % |
4.8 % |
|
IVF without ICSI |
30.2 % |
21.2 % |
12.9 % |
6.5 % |
1.6 % |
| Age | <35 | 35-37 | 38-40 | 41-42 | >42 |
|
Miscarriage Rate After Clinical Peegnancy |
12.7 % | 15.3 % | 18.0 % | 22.2 % | 35.0 % |
IVF Miscarriage Rate
These percentages are miscarriages per egg retrieval, for patients going through their first embryo transfer. As we can see, miscarriage rates almost triple from the youngest age group to the older age group. According to this data, for women over the age of 42, 9629 cycles were started. Around 606 of these cycles resulted in clinical pregnancy, and around 212 of these pregnancies resulted in a miscarriage. As we learned, older patients have fewer eggs rthat are of poor quality, and their pregnancies significantly have a higher risk. They have a harder time attaining pregnancy and sustaining it. [1]
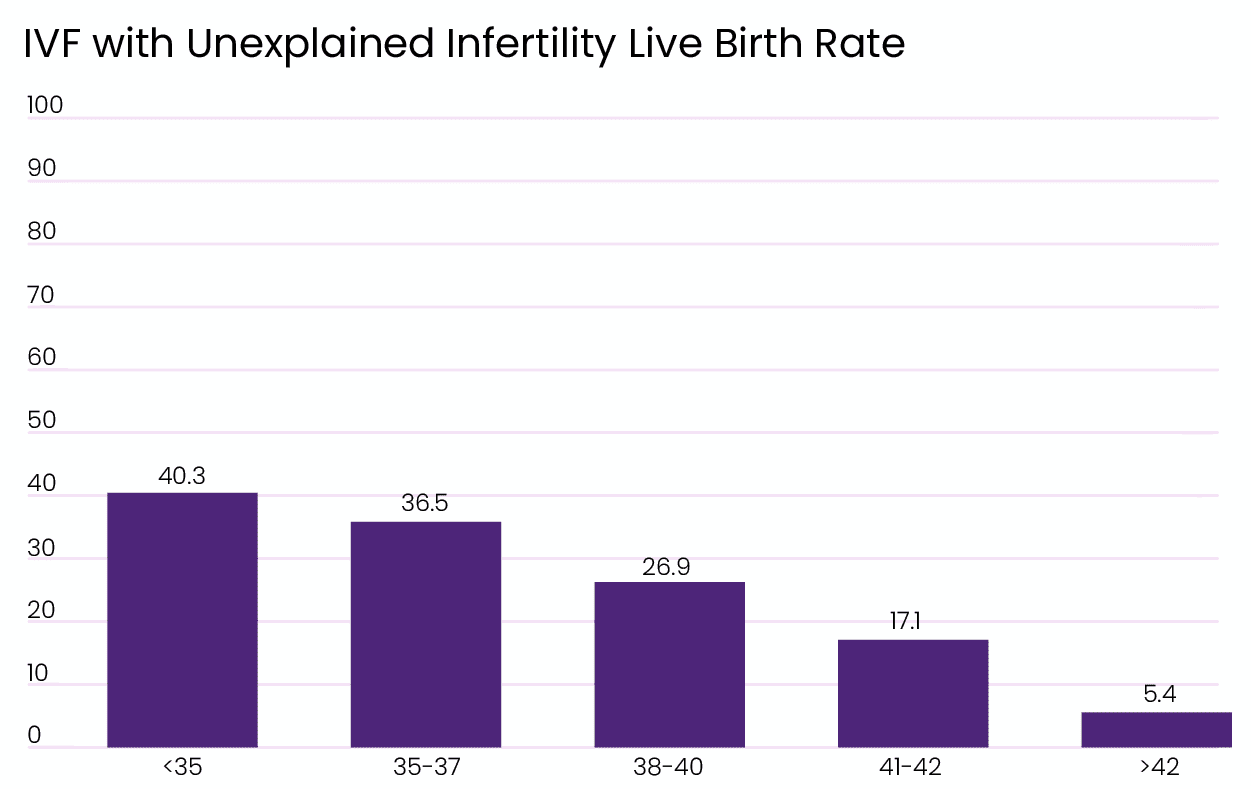
Unexplained Infertility IVF Success Rates
For patients suffering from unexplained infertility, success rates are also similar to all diagnoses. The diagnosis of unexplained infertility can be disheartening. It’s difficult for patients to accept that science cannot find a reason for their fertility problems. Even though the causes cannot be pointed out, IVF is the best treatment available for unexplained infertility. [1]
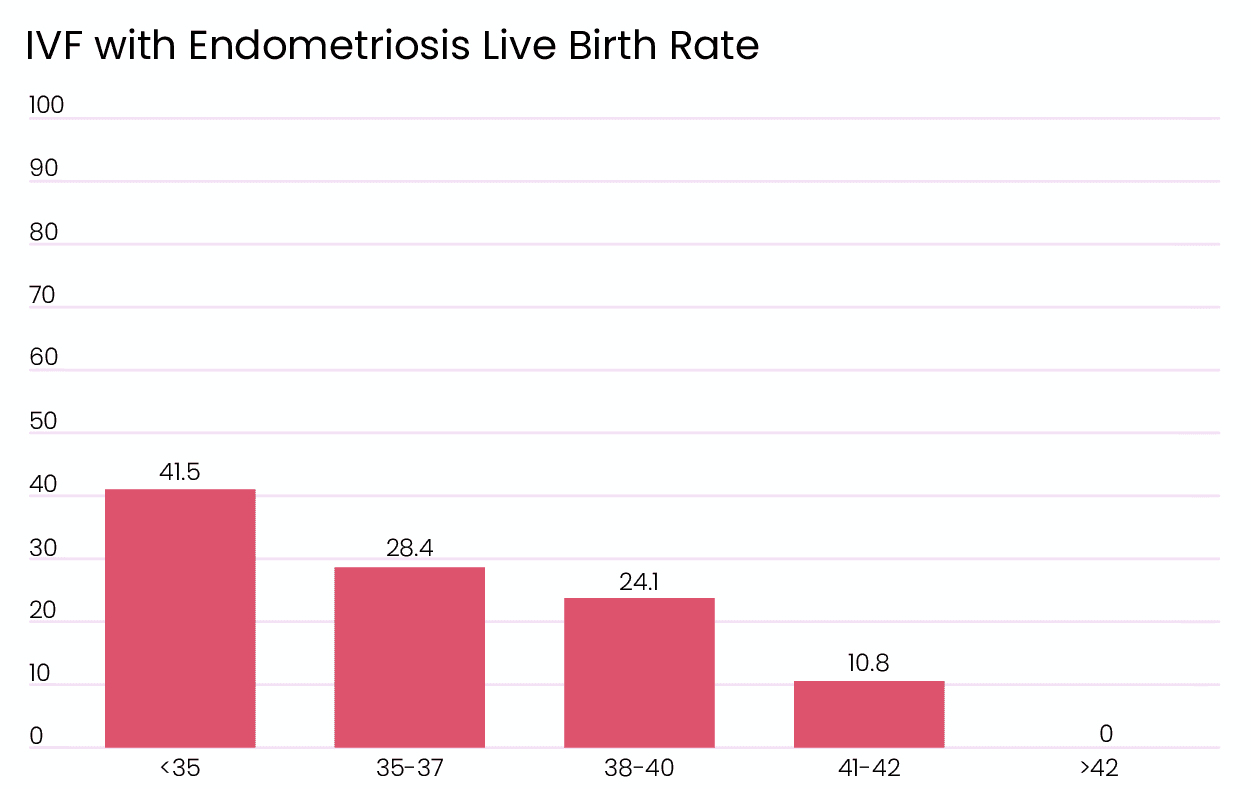
IVF Endometriosis Success Rates
Most patients who have endometriosis can think that they can never get pregnant, which is wrong. IVF combined with other endometriosis treatments can allow patients with endometriosis to get pregnant. The success rate for live births with endometriosis is only slightly lower than IVF for other causes of infertility. The data for patients over the age of 42 was very, limited with only 39 cycles performed. Out of 39 of those cycles, 1 ended up in a clinical pregnancy that unfortunately resulted in a miscarriage. [1]
IVF After Tubal Ligation Success Rates
A lot of women who had their tubes tied in their youth turn to IVF to get pregnant. IVF bypasses the natural conception process that happens in the fallopian tubes. Thus, women who previously had their tubes tied, or women with blocked fallopian tubes can get pregnant through IVF.
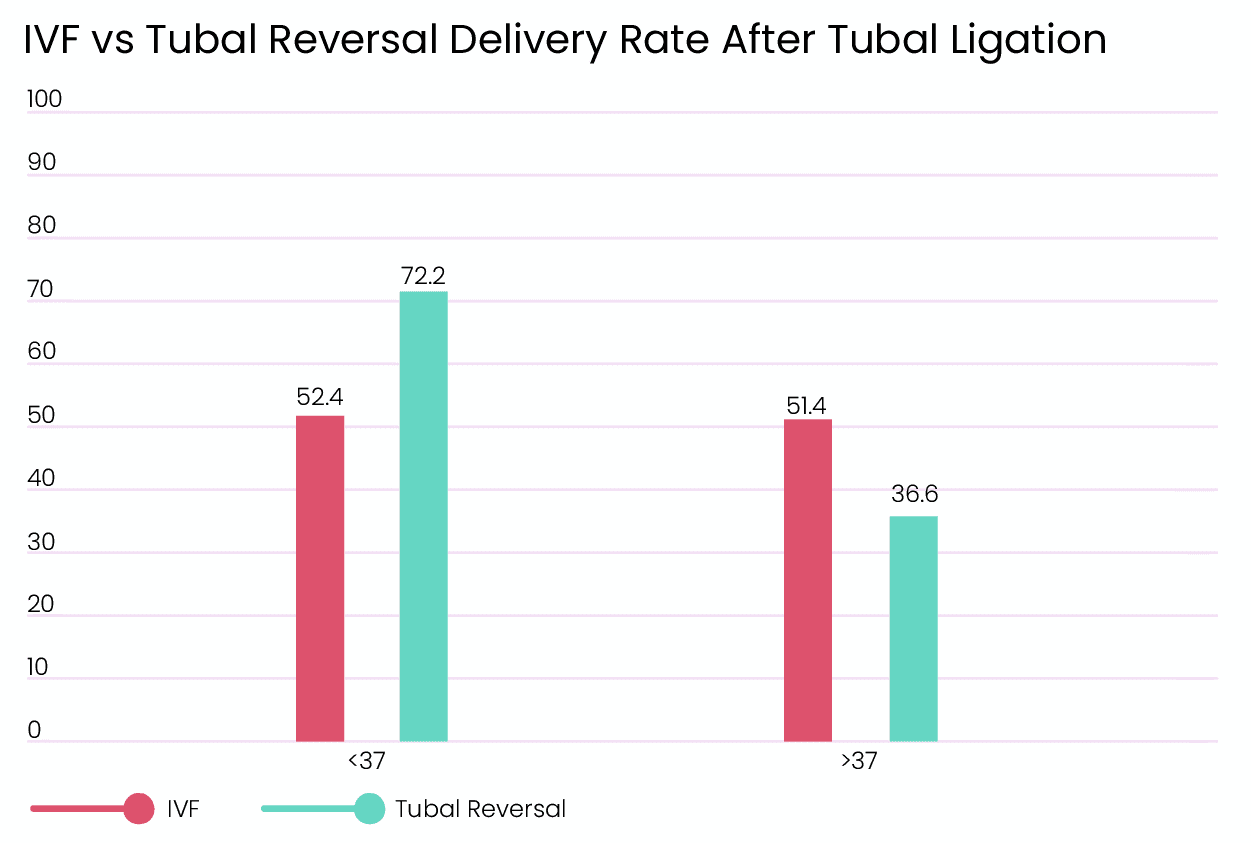
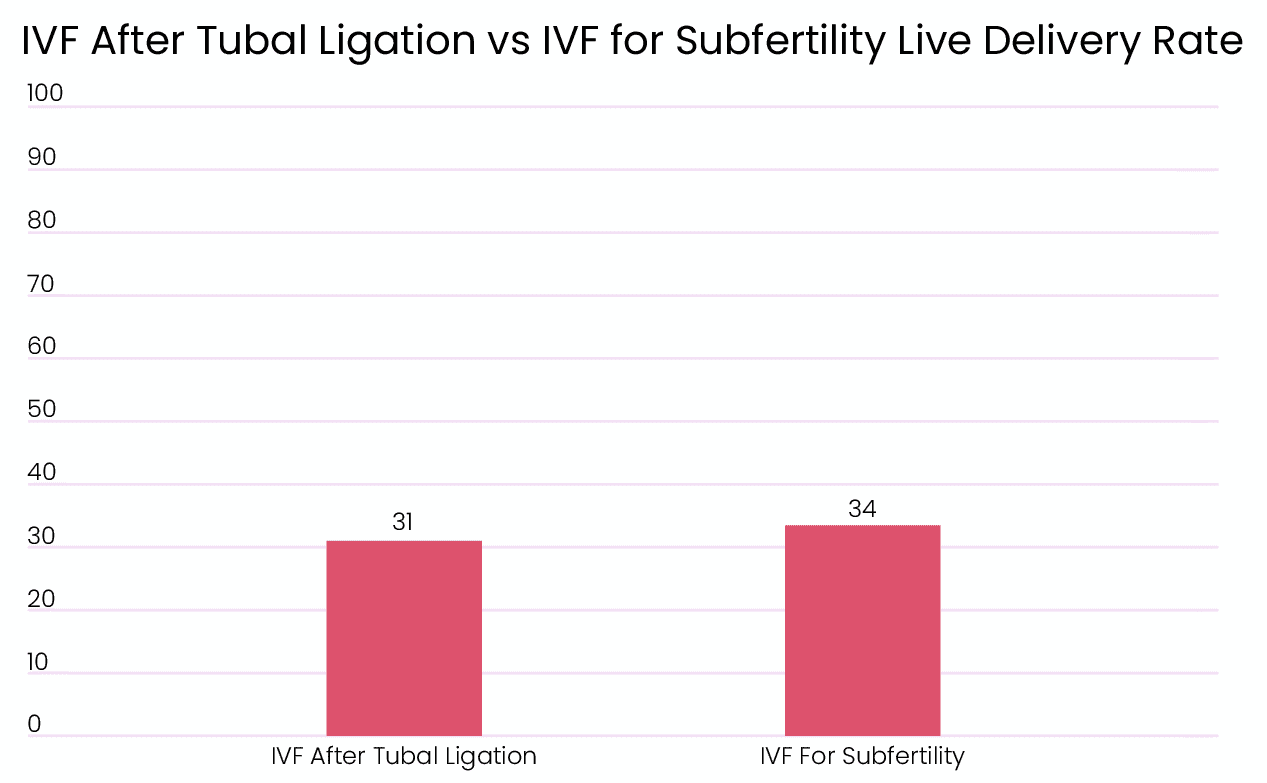
Tubal ligation can be reversed with surgery. But some patients might not want to go through another round of surgery and opt for IVF as their first course of treatment. In cases where the patients or older, IVF after tuber ligation is more successful than reversal. However, younger patients can still opt for reversal as it can provide higher success rates. [3] The success rates of IVF after tubal ligation is similar to the rates of people with other subfertile patients. [4] Rates for younger women were also on par with the subfertile group, but live delivery rates declined with age. [4]
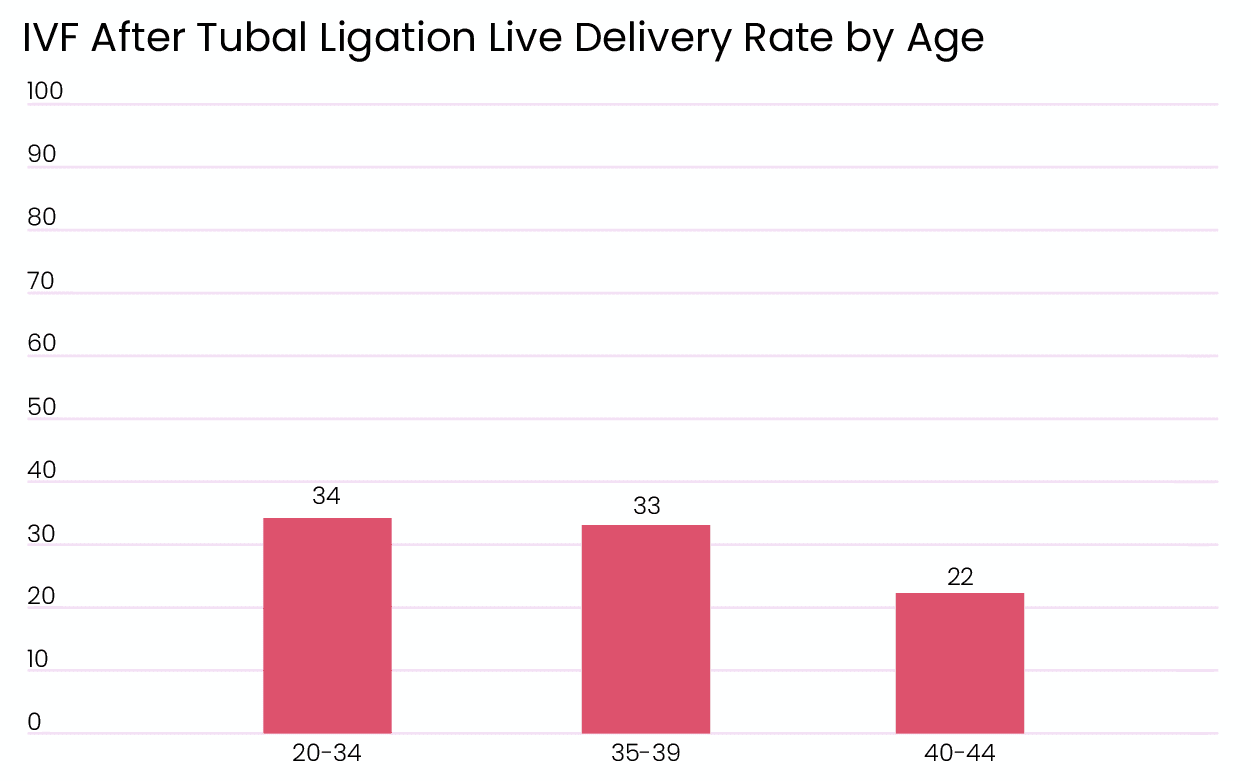
How to increase IVF success rate
When it comes to increasing the live birth rate with IVF, there are a lot of Assisted Reproductive Technology options to help patients. These procedures or technologies can help people who are having difficulty because of certain issues like abnormal embryos, implantation, etc. Let’s go over these procedures one by one, and how they can increase success rates. If you’re interested in how you can increase your success rates through diet and exercise, you can check out our IVF lifestyle guide.
IVF with PGT Success Rates
Another common procedure employed during IVF is PGT. Pre-genetic testing allows patients to test their embryos for genetic diseases. With PGT, parents that are a carrier of a genetic disease can avoid passing the illness down. Or, patients that are having recurrent miscarriages, or IVF failure can try PGT to improve their results. To see the effectiveness of PGT let’s look at live birth rates when PGT is and isn’t used.
|
Age |
<35 |
35-37 |
38-40 |
41-42 |
>42 |
|
IVF with PGT |
46.0 % |
39.3 % |
30.1 % |
18.7 % |
7.9 % |
|
IVF without PGT |
36.9 % |
23.9 % |
13.8 % |
5.9 % |
2.0 % |
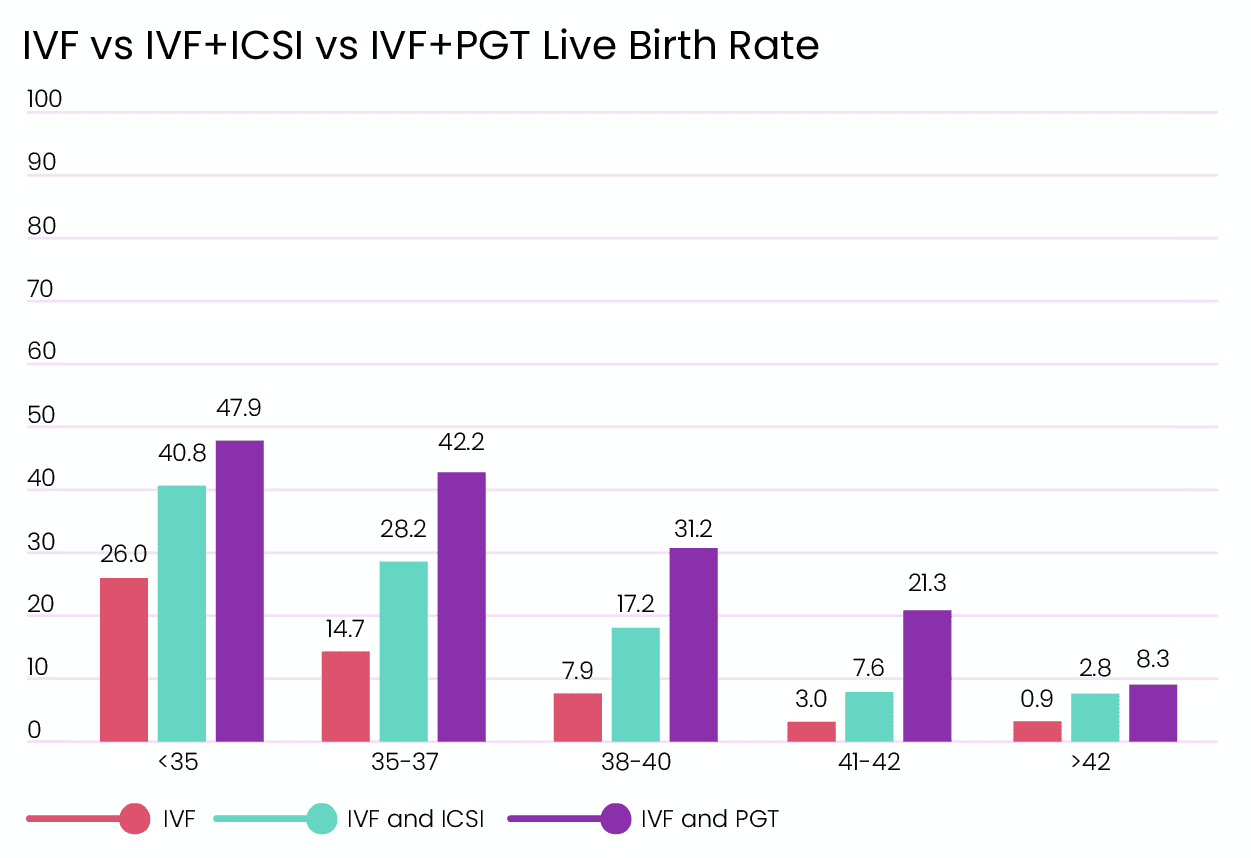
According to tot the data, when PGT is used, the live birth rates can be 4 times higher compared to when it’s not used, especially for older patients [1]. Now, let’s compare some live birth rates when these adjunct procedures are used/not used.
IVF on its own has lower live birth rates. But when IVF is used with ICSI or PGT, it has significantly higher chances. Especially for older patients who have low-quality eggs and embryos, PGT is extremely useful in choosing a viable embryo and can improve the chances of live birth up to 8 times compared to IVF on its own [1].
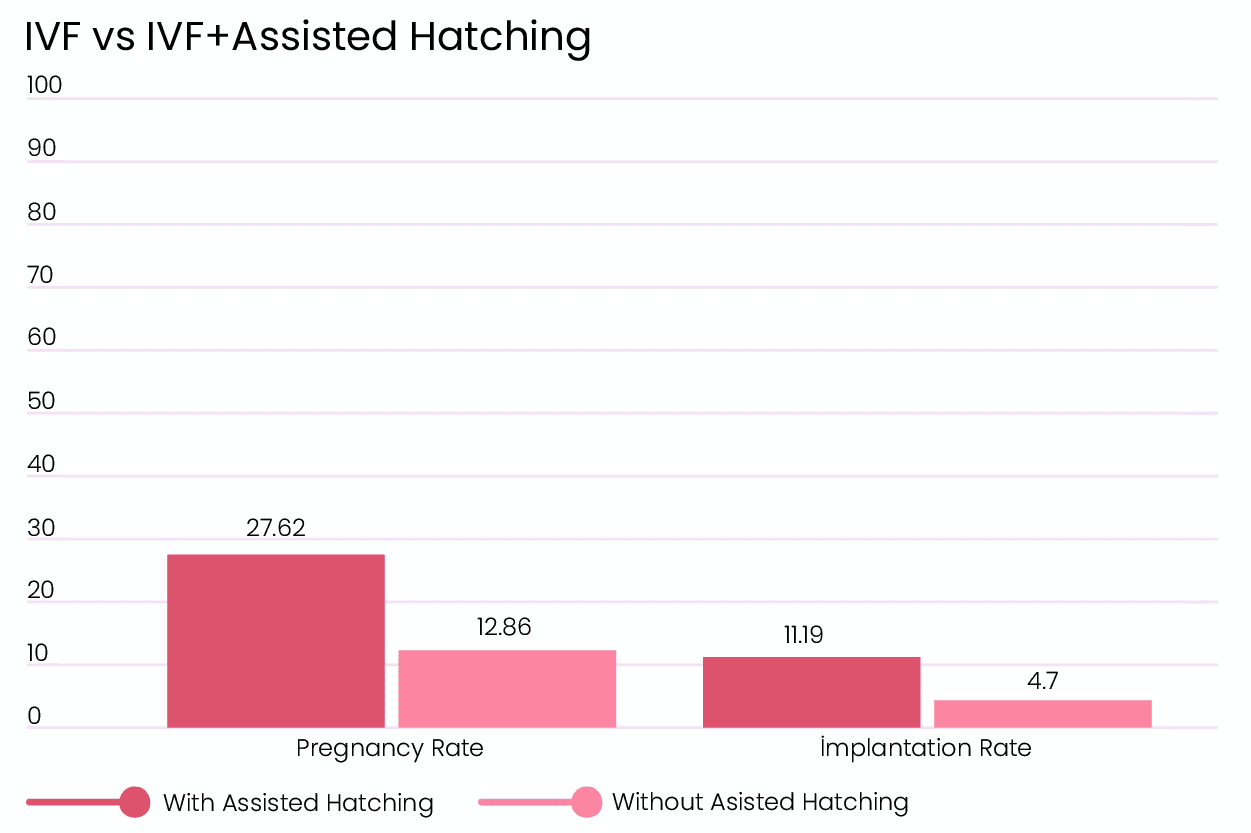
IVF Assisted Hatching Success Rates
In this paper where multiple AH studies were analyzed, Assisted Hatching can improve implantation rates, especially for patients over the age of 38, presenting with poor prognosis or oocyte quality, and having had multiple failed IVF cycles. [5]
What is assisted hatching in IVF?
Assisted hatching is a technique where a small part of the outer layer of the embryo is mechanically or chemically thinned out or removed. The egg has an outer layer called Zona Pellicuda. During fertilization, the sperm enters the egg through this coating. To prevent the entrance of another sperm cell, the Zona hardens after fertilization.
Assisted hatching can be performed mechanically, or chemically. Mechanically, the zona is scraped and thinned. Chemically, enzymes are used to dissolve and thin out the zona. Today, most AH procedures are performed with a laser. This method is preferred because of its precision, and it’s minimally invasive to the embryo, keeping it intact and healthy.
When is assisted hatching done in IVF?
The hardening of the zona can make it difficult for the blastocyst to hatch and implant properly. The zona pellucida can harden due to advanced maternal age, in vitro culture conditions, and cryopreservation [6]. In cases where zona hardening is present, assisted hatching can help the blastocyst to separate from the zona, and implant in the uterus.
IVF Embryoscope Success Rate
Embryoscope is an incubator with a built-in camera that constantly monitors the growth of embryos. After insemination, the fertilized egg is put into Embryoscope for incubation. IN a regular incubator, there is no camera constantly recording the embryos. By recording the embryo development at all stages, Embryoscope allows us to watch, predict, and learn from their development.
Embryoscope is most useful when it comes to the selection of normal-looking embryos. In addition to this, patients can ask for the recordings, and watch their embryos growing.
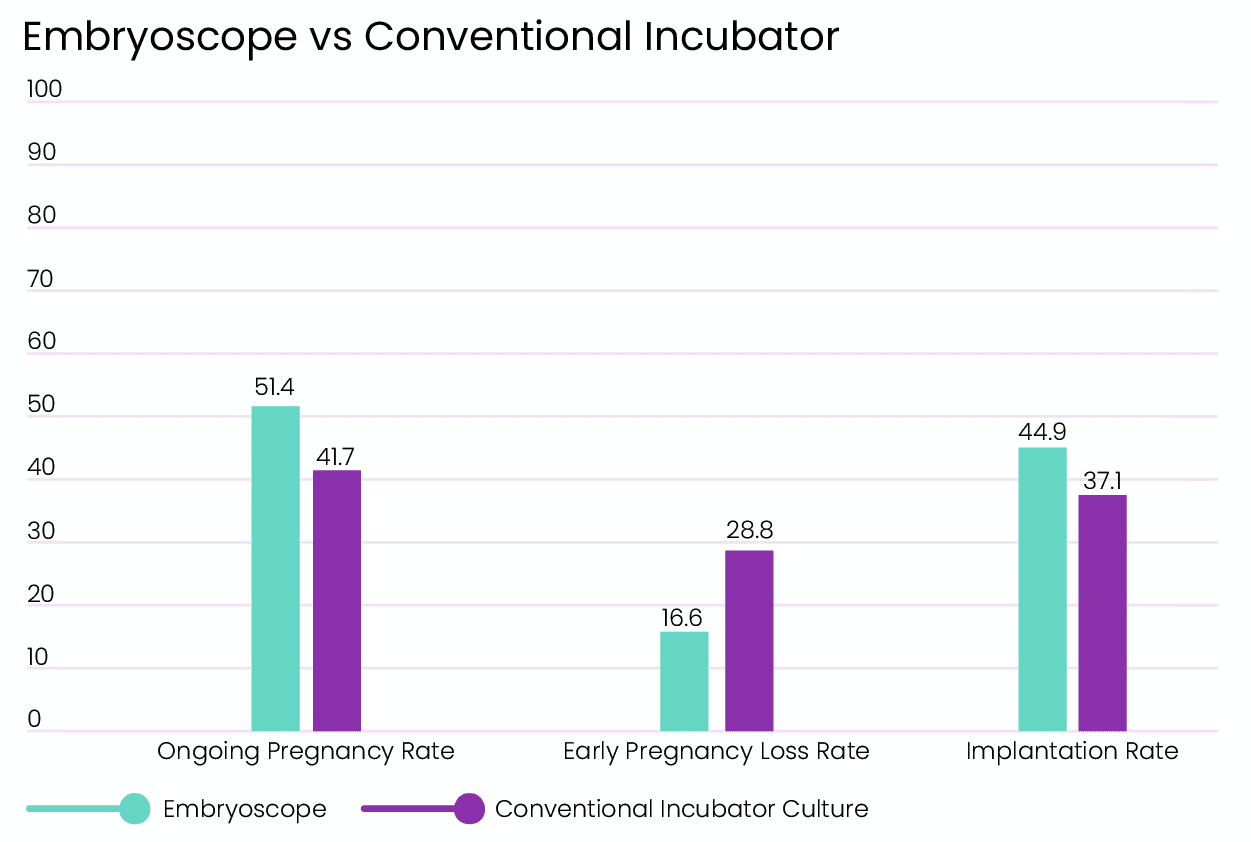
Embryoscope is more than just a fancy incubator with a built-in video camera. Because it allows the doctors and the lab to choose the best embryo, it improves success rates greatly. In a study, it was found that using Embryoscope instead of a conventional incubator, and choosing the best embryo available significantly increased implantation and ongoing pregnancy rates. It also significantly reduced early pregnancy loss rates [7].
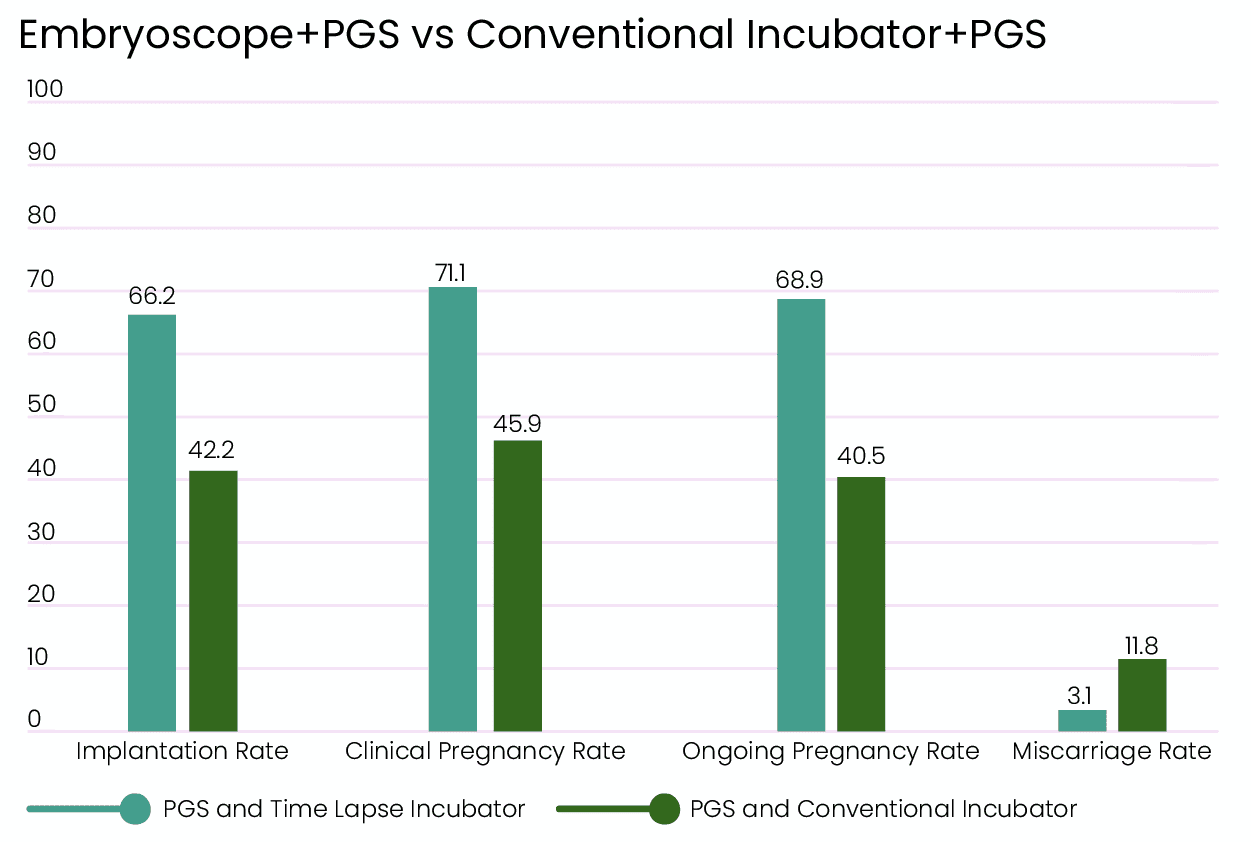
Where Embryoscope makes an impact, is when it’s combined with PGS. This allows doctors to choose the best embryos that are normal, and healthy. This helps to improve implantation and pregnancy rates compared to conventional incubation methods where embryos can’t be monitored constantly [8].
You’ve reached the end of this chapter! Now you’re up to date on the latest data when it comes to IVF. You probably have some idea of what kind of results to expect, and which adjunct procedures you want to have during your treatment. For now, let’s have a little break from what IVF can do for you, and move on to what you can do before IVF to get the best results possible.
